Scar Revision
As a plastic surgeon working in New York City I see all manner of injuries and surgical scars in every type and color of skin on this earth. Most times scars heal well or at least don’t bother patients. Occasionally however, the mark left behind is either in a particularly bad place (like the face) or heals with an unacceptably bad scar. These scars may not only be ugly to the observer, but can sometimes affect the functionality of the patient by causing constriction in movement (especially across joints). This is where the art of plastic surgery might be appreciated by even the most staunch opponents of plastic surgery.
Why Do Scars Heal Poorly?
This is one of the key questions of surgery and we may never get a 100% complete answer. Wound healing is clearly genetic to a large extent with some people being more prone to making thick scars than others. For instance, African American patients who come to my office are very cautious about their chances of producing a keloid scar (a scar that extends beyond the borders of the original injury). Interestingly, my experience has been that the Asian population is at greater risk of keloids than anyone else. That doesn’t mean that everyone in these populations makes poor scars, but when I do RARELY see a keloid, it is many times in one of these ethnic groups.
Beyond genetics or God’s will, there are environmental influencers of scar formation. For instance, if a wound was infected it may very well form a bad scar. Infections will many times lead to thickened scar tissue, wounds that open up and have to heal from the inside out, or scars that are tethered (stuck) down to the underlying tissues of the body creating divots or dents. If a wound is closed under tension, the body seems to react to the need for more aggressive healing by depositing more collagen in the area leading to a thicker scar. Treatments such as a melanoma cancer treatment can also cause scaring. There are also parts of the body that are known to be more likely to create bad scars. The center of the chest, the earlobes, and in my experience the upper arm all fall into that category. All of these factors create a more obvious and less appealing scar long term.
Keloid Vs. Hypertrophic Scars
A “keloid” scar is a scar that grows out beyond the borders of the original wound. They are a terrible problem and can be very tricky to get rid of because once you have one, there is always a risk that any attempt to remove it could result in another keloid that is worse than the first one. There are a handful of treatments for keloids including the injection of steroids, anti cancer drugs, and even radiation therapy. The best results seem to require excision of the keloid with the immediate use of one of these adjuvant therapies. The theory is that by limiting the earliest wound healing processes (what doctors call an influx of “macrophages”) we can prevent an overabundance of collagen deposition in the area.
A “hypertrophic scar” in contrast to a keloid is simply a scar that is a little thick, or that we don’t particularly like. I have many patients who tell me about how they “keloid” when in fact they simply have a hypertrophic scar. Luckily, the treatment of a hypertrophic scar is a whole lot simpler than that for a keloid. Many times I will simply give the patient an injection of steroid and the scar settles down pretty quickly. Other times we go to any of the other treatments that I’ve described in this writing with good outcomes.
Vitamin E Is Bad For Your Scar, Silicone Gel Is Good
Plastic surgeons and dermatologists have known for years that vitamin E is bad for the cosmetic healing of scars. Vitamin E is proven to decrease the tensile strength of wounds and produce less favorable scarring than doing nothing at all. I’ve been telling patients this for years, but most don’t really believe me because their mothers, friends, and sometimes television tells them otherwise. It’s an uphill battle, but I keep trying.
In my practice, I suggest the use of silicone gel as an effective method to improve the appearance of scars. This is supported with real clinical research both on the laboratory bench and in clinical studies. Actually, silicone sheets are also very effective, but I find patients are more likely to stick with the gel because it is much easier to use. Patients tend to complain about the sheets and they become very expensive over time as repeated use seems to make them somewhat “dirty” and patients don’t want to use them after a while. The gel is simple, dries fast, and patients are more likely to stick with the regimen for the 6 to 8 months required to really make a difference.
Basic Scar Revision
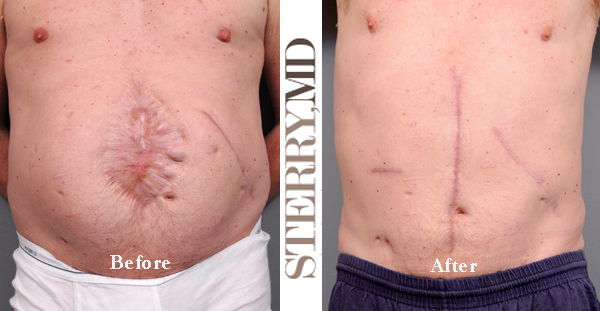
Sometimes the most obvious thing to do with a bad scar is simply to remove the bad scar tissue and close the wound all over again in a very similar manner. This can work out well, depending on the situation. That is, one has to ask oneself why the scar is likely to form more favorably on the second go round than the first. For instance, were the wound edges lined up properly the first time? Was there some kind of contamination or infection that caused poor wound healing? In those cases, a simple scar revision can certainly result in a more acceptable cosmetic appearance of the scar.
Sometimes there can be too much tension on the closure of a wound the first time around which caused the body to react profoundly and deposit a lot of collagen in the area causing a thickened scar to form? If the surgeon can somehow relieve that tension (perhaps by creating a “flap”), then the outcome might be better the second time around as well. This situation comes up all the time in cases like bad tummy tuck scars or after general surgery.
Z-Plasty Can Help Release Constricting Scars
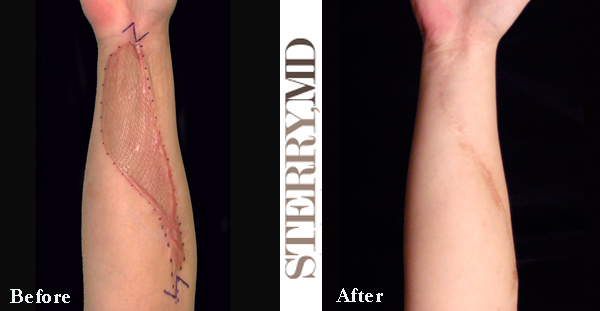
If a scar crosses a joint like an elbow, knee, or even your neck there is a procedure called a “Z-Plasty” that can help to release the constriction by recruiting some non scarred surrounding tissue into the central portion of the troublesome area. There are times when this makes the scar more cosmetically acceptable, but generally speaking this technique is used to restore function to the patient. It is a commonly utilized strategy in hand surgery (because there are so many scars that cross joints in that field) as well as burn surgery (because these wounds tend to be large and cause great constriction. However, Z-Plasty is used in any situation where we need a little tissue rearrangement.
W-Plasty to Help Camouflage Scars
W-Plasty” is similar to a Z-Plasty in that we create a zig-zag scar, but in the W-Plasty the zig-zag is continuous along the length of the scar. It is particularly useful in scars that run in the opposite direction as the natural lines in the body or face because we can take (for instance) a vertical scar and create a series of smaller 45 degree angles that are closer to the horizontal lines we normally find in nature. This seems to throw off the eye of the onlooker so that the scars is not quite so noticeable. That is, the wound runs opposite to the normal creases we would see naturally, but the series of smaller scar lines are now 50% closer to them. It is a very handy procedure in the right circumstances, but patients in general are reticent to the idea because they are afraid the wound might look more like the mark of Zorro than a better scar.

Dermabrasion to Help Scars Blend In
Once a scar has been optimized by any of the other methods described here, we still have a few techniques that can help scars to “blend” into the surrounding skin. One of these is called “dermabrasion“. This is a technique that essentially uses a small grinding wheel as a handheld device to physically file down a scar and the normal tissues immediately surrounding it. By removing the top layer of skin in these areas we cause the entire area to heal or “re-epithelialize” in unison and that can help the scar to be less noticeable. It is very effective and handy. Plastic surgeons like this technique for getting rid of wrinkles around the mouth that a facelift can’t quite achieve. Sometimes dermatologists will try to cover large areas of skin like the cheeks after acne scarring and they call this “derma planing”. Amongst the limitations with this procedure is that it is very user dependent and difficult to get large areas of skin to be completely uniform.
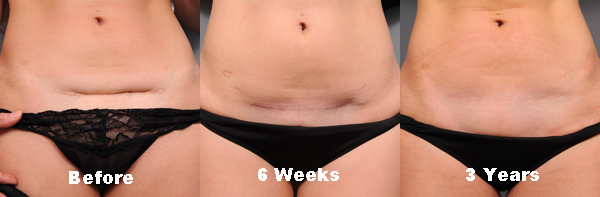
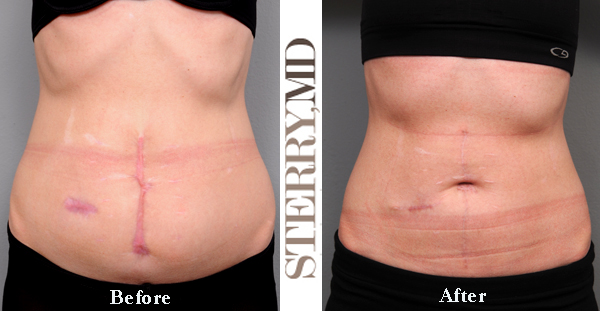
Complete Removal of a Scar
To say that we can “remove a scar” is sort of a misrepresentation of our abilities. Once a scar has been formed, it may fade with time, but it will never completely “go away”. On the other hand, we do have the ability to remove one scar and “trade” it for a different one… and this trick is worth doing from time to time. For instance, perhaps there is a vertical scar on the lower tummy of a woman after having a Cesarean Section (“C-section”). We certainly have the ability to remove all of the lower tummy skin and convert the “up and down” scar, which is visible to the whole world, to a gentle horizontal “smile” scar across the lower bikini line with the use of a classic tummy tuck procedure. The only visible scar to the public would be around the umbilicus and I’ve written quite a bit about that issue in my other posts. Other examples might include any number of breast procedures or thigh lift operations – all of which involve removing skin which, if scarred, would eliminate an unfavorable scar for a more cosmetically acceptable or hidden scar.
Laser Treatments That Lessen Scars
There are several types of lasers that can be helpful in our battle against scars. These can be categorized as Ablative, Vascular, and Fractional Non-Ablative lasers.
Ablative lasers can be used in much the same way as dermabrasion. They essentially sear the surface of the skin and take away the surface level of skin in the hopes that when the scarred area and surrounding tissues heal they appear more uniform. The advantage over derma planing is that these devices are less user dependent and results seem to be more reliable when treating large surface areas – as with acne scarring.
Vascular lasers help to remove redness from scars. They use a specific wavelength that is absorbed by the red color and essentially burns it out of the area. The result can be a scar that is less red, and hopefully has a pigment more like the surrounding skin.
Fractional Non-Ablative lasers are not supposed to take away the skin surface, but rather they deliver heat down into the scar in micro “tunnels”. The theory is that they can burr thousands of microscopic holes of heat into the scar and encourage the skin to heal again in a more uniform manner. While the idea is inviting, I have not been impressed with this technology in my practice and have completely abandoned the technology for now.
Injections to Improve the Appearance of Scars
There are some occasions when injectable materials like Juvederm can help scars to look better. For instance, let’s say that there is a depressed scar that looks like a dent in the skin. It may not make sense to operate because the scar is so small and we want to do as little as possible to get a favorable outcome. So in these cases we can sometimes inject a little filler under the scar to make it “pop” up to the same level as the surrounding surface skin. When it works, it’s a home run, however fillers are a little pricey and the results may only last a year or so (based on the longevity of the filler). For these reasons I typically will check to see if I can get the scar to pop by injecting saline first. If the scar is not tethered down to the underlying tissues it will smooth out, and then I know that a filler can help. On the other hand, if the scar won’t budge because of the connections below, then I know that I need to try some kind of lysis (sub dermal release of the scar). This can sometimes be achieved with a needle or a device such as a “diamond wire” that is specifically designed for “subcision” of the scar.
Will Insurance Pay for Scar Revision?
Your health insurance company is supposed to be there to help pay for “health” or medically necessary procedures. As such, insurers are not exactly going to leap at the opportunity to help you get a cosmetic scar revision. However, if a scar is actually preventing you from leading a healthy and productive life, then they may. For instance, if there is a scar restricting movement of your hands or arms so that you can’t work, then a scar revision would be deemed “medically necessary” and your insurance carrier would likely pay for that kind of revision. On the other hand, if a patient doesn’t like the appearance of your acne scarring, that is probably going to be considered an elective cosmetic procedure and the expense would be on the individual. The tricky part here is that some insurance companies will deny any and all scar revisions because some patients will make claims about their inability to work due to a cosmetic scar – so there is definitely a struggle in many cases to determine what is fair. As a plastic surgeon, I do my best to walk the line between these opposing views. I want what is best for my patients and I advocate for them every day, but sometimes we need to concede that a given procedure is simply cosmetic in nature.





Do u do out of state consultations? Like via skype? I have a cheek scar from a mole removal as a child that i have had revised but still very unhappy with how it looks…
Yes. Please call my office at (212) 249-4020 and we can set that up for you. I look forward to meeting you!
I was definitely botched and I would love
to know how much the procedure cross
Please email me
Did you ever send us pictures?
[email protected]
I am seventeen years old and I have scars on my breasts from picking. I was wondering if you could do something about that. Please let me know, thank you.
I would love to help you out, but would need to see what you are talking about. If you are in the New York City area, perhaps you can have your guardian bring you in for a consultation. Sorry, but I can’t have someone younger than 18 send photos to evaluate. I hope you understand.
I have an almost identical C-section scar as the one of the 29 year old above. I’m 40, in good shape but just don’t like the way it looks or feels. What is a rough estimate of cost in fixing that scar like above in the pictures? Thanks for any information
I don’t ever speak about money, but you can certainly email my office at [email protected] and they will discuss that with you. Would love to fix it, whatever it is!
I have few scars on my knees and I will Like to know if there is Something you can do to reduce the appariance of them
Knees can be tricky. Why don’t you send us some photographs and I will let you know what I think?
[email protected]
I am an 18 year old male and I have a vertical scar on my abominals from a surgery i had on my spleen when i was 12 years old, I was wondering if I could send some pictures to see if you could help, Please let me know, Thank you.
I would be happy to have a look.
Send photos to [email protected].
I will let you know what I think.
HI Bryan,
I’m 34 and had a splenectomy performed 4 years ago. I had 8 sessions of laser treatment which improved the appearance of the scar but I’m still conscious about it as it’s still pretty visible. Have you had any treatment/ surgery that has worked?
A Splenectomy is a significant operation, and if it was performed using an open technique…yes, I can understand your concern. That said, your question is very fact based – so I’d need to have a look at it to tell you if I think non-invasive treatments are going to help or not.
I have ingrown hairs in my pubic area, years of picking have left VERY visible scarrinh. Is that something I can removed?
That’s kind of a tough one and depends on exactly what you mean. Can you send photos to [email protected]? We will get back to you quickly.
That really depends on the scenario. Can you send photos to [email protected]?
Hi my name is Ali for the past three years I have had scars on my upper arms and thighs. It spread I’m sure of it I have no idea what caused it no dermatologist has been able to give me a straight answer it keeps me from living a normal life I can’t wear the shirts or shorts it is red and all over it looks like a rash a bad one that never went away I’m desperate. Can anything be do e to make the skin on my arms and thighs look normal again???
I would need to see what you mean. Why don’t you send some photos to [email protected]?
I will have a look at them personally and we will get back to you.
About four years ago, I used nair all over my pubic area and it burned me. So now I’m left with these little and big hard bumps. I went to a dermatologist who told me it was just folliculitus, but I’m sure it’s scarring. Do you think that I could have all of the scarred, bumpy skin removed?
And if i do get it removed, will the surgery scar be able to be hidden in a crease?
The scar is typically along the bikini line like the other tummy tuck scars we do. I personally try to make mine neat and in an area where nobody is going to see them except your dog and lover 😉
I would have to see what you mean, but it doesn’t sound like a great idea to remove the mons pubis. Furthermore, don’t forget that we would need to make a scar to remove the existing scars…
The scars are on my labia majora
Oh Dear! That is unusual. I think photographs would be inappropriate. I encourage you to see your gynecologist for that area. Good Luck!
Hello Dr,
I have a decent size Keloid on my upper chest, it’s over 10 years old but I tried to have it removed by a dermatologist back in 2014 (poor decision) and it came back with vengeance. I’ve been getting injections for over 7 years and it’s only a temporary fix. I am ready to try removal again but with a more knowledgeable Dr.
Hello my name is Shawn and I would like to look into the scar Removal program
okay, how can we help? Would you like to send me a photograph so we can talk about it?
I have an indented appendectomy scar that causes me pain and makes it harder to exercise. As I’ve gained weight it’s become more indented and is stretching the other skin to the point where there’s huge blown out stretch marks all around it. I don’t mind having a scar, just hate that one side of my stomach is unbalanced and indented, and that it hurts a lot of the times.
Yes, I’ve seen that exact scar scenario before. That nice part is that having fixed it a few times, I feel like it’s kind of straightforward now.
Hello,
I recently had surgery to removal a hernia mesh and repair my abdominal walls. Now my stomach is disfigured without a belly button. Am I a candidate for scar revision?
Sounds like you may need an abdominal wall reconstruction. My colleague David Chessin and I do a lot of these. It’s a little bit of a hobby for us and we really like putting people back together.
Hi.. my daughter was burned with hot water on her right upper arm when she was 1 year old, she’s now about to be 15. They did skin graft and we would like to know if something can be done to reduce her scar before getting her hopes up. Thank you doctor.
Actually, I just did one like that over the last few months. We were able to remove the entire skin graft – although I must say that this was an adult patient. Many times this can be done as a “serial excision”, but sometimes a tissue expander is helpful.
I have a small nevus (approximately 1cm diameter) on my chin that has been removed by shaving method on multiple occasions only to regrow. I had it addressed with laser over a decade ago however there is still a raised area, hairs sprout from the area and it frequently scabs over in the fall/winter whenever my skin is dry. I have finally decided enough is enough and I would like to have it excised however I am concerned about the issue of scarring. I wonder if you have any suggestions for surgical options, approaches, or considerations that would reduce appearance of scarring. Thank you in advance.
All I can say is that you’ll need to have it completely excised (down to the “root”) and then closed nicely. It will be fine at first, turn red for a while, and hopefully fade by about 9 months.
Good Luck!
I am 12 weeks post partum after a c-section (and live in kansas city). I am unhappy with the way my scar has healed—lumpy on one side with what feels like a roll of fatty tissue on my otherwise not fat stomach… can you do a consult via facetime/photos? I am wondering if i need to give it more time to heal or if i should get it fixed. I have looked at your work and want to come to you!
I would be happy to chat with you about your situation. Please email us at [email protected].
i have a bad indented c setion scar that us very recent only 41 days old but im very consern because it has heal with indentation on my left part. and now my stomach looks bigger in the left i have send you the pictures through email
At barely 6 weeks post surgery, I would not rush to change anything about your C-section scar. You would be surprised how much things can change with a little time. Please give it 6 months and then I’d be happy to discuss.
How difficult would scar revision at the top of my butt crack be? I have a surgical scar and I was told it was high risk.
I suppose I would need to see it.
I had a broken blood vessel, right between my eyes, “zapped” by a laser and it has left a divoted scar- I’ve since had 3 Smooth Beam laser treatments; the last one causing the skin to burn off. 2 weeks later, the skin has healed but the divot is still there. I’ve been sick over this- been dealing with this March 2017…prior to Smooth Beam, I had 2 injections of fillers. Any suggestions of anything that might help?
Sounds like you’ve already tried a few non-invasive techniques. Maybe it’s time to either revise the scar surgically or do a little subscission followed by a filler?
wow impressive, what gifted hands may God continue to bless them..
unfortunately i live in Australia…:(
I had a bilateral masectomy. On my left side I have a horizontal scar…the problem is, that one side has been heavily radiated and under the scar is my stretched marked stomach as my breast (I had a tram flap procedure) any suggestions?
Stretch marks are tough. I think you need a local surgeon to have a look. I’m sorry I can’t be more helpful…this sounds like a tough one.
Good Luck!
Hi,
I have a brand new (10 days old) indented scar under my chin after falling and getting 3 stitches. What would you recommend I do for it for now? Is it ok if I start putting mederma on it now? I am guessing it is too early to get any type of filler or laser.
sorry for such a late reply! I missed your question somehow.
I’m not a fan of mederma for scars. The only thing proven to improve the appearance of scars in a laboratory and under controlled conditions is silicone (gel or sheets).
How is it coming along???
I had a basal cell removed on my upper arm. I was very unhappy with the result. I had a consultation with a local plastic surgeon who was very optimistic that revision could improve the appearance but when I arrived to have the surgical revision procedure -he seemed to be less optimistic. I am worried I’ve made a mistake and it will look worse. Do you have any tips for optimizing the healing results?
The shoulder area is a tough zone for scars. I’m not typically in a hurry to revise anything above the deltoid. Sorry if you feel like your surgeon disappointed you.
Good Luck!
I have hundreds of small scars all over my lower arms from the inner elbow to the wrist and thighs from the hips to the knees. I can’t wear shorts, skirts, short sleeves, dresses, or go to the beach because I don’t want anyone to see them. They’re normal scars, no keloids or extreme hypertrophy, but they are slightly raised and much whiter than the surrounding tan skin. Should I get laser removal? Would it be pheasible for so many scars?
Sounds like the laser is your best bet. Try a local board certified dermatologist.
Good Luck!
What is the best option for a dark tummy tuck scar? I’m caramel complexion and the scar is dark chocolate in most areas.
I would recommend silicone gel and perhaps a retinol – but you need to have a local physician have a look first, I don’t know anything about your skin and have never examined you.
Good Luck!
Can I send you a picture of my scar and tell me about what you think would be the best approach for my to take with my arm. I’m already seeing someone about my scar I’m just welcoming another opinion.
of course!
[email protected]
Is it best to get scar revision soon after the wound heals, or earlier, or is best to wait until longer-term healing has taken place? I cant’t seem to answer this with my own research.
Do you think insurance would be likely to pay for a scar revision procedure for scars caused by a medical emergency and a resulting medically necessary surgery that were both caused after serious complications during an orthopedic surgery?
There are 4 scars along my ribs and latimus dorsum caused by large medical tubes. The tissue is sore and tight, and for now the scars/ holes constrict my movements of stretching and rotating my trunk.
Thank you considerably for your time, Doctor. I recognize that questions about insurance charges are outside the scope of your work.
Personally, I like to wait at least 6 months. More than a year seems unreasonable – you either know it’s going well or it isn’t.
I have scars on my upper arm, they are from deep cuts and are purple, with smaller white scars around them. What can I do?
The specifics are really important.
You can send us some photos if you like…
I have a vertical scar from my diaphragm to my pubic bone and I have no belly button at all after a botched trans flap reconstruction (breast cancer) I had to have a hernia specialist repair my abdomin to give me abdominal support. I’m just wondering if there’s anyway to construct a new belly button.
I am 100% sure we can reconstruct a new belly button.
https://www.drsterry.com/photo-gallery/body/scar-revision/146/36
Please call my office: (212) 249-4020
What would you do for scars on the stomach from an organ transplant? Or a scar from a feeding tube?
The “Chevron” incision from an organ transplant can be cosmetically devastating. Also, the feeding tube scars tend to get tethered to the underlying tissues and can certainly be disturbing – as small as they are.
The answer to your question really depends on the exact scenario and what a given patient needs…
Hello Dr.Sterry,
I live in NY, I am 26, and I’m scheduled to get a right hepatectomy using the Makuuchi in the next few weeks. I was told laparoscopic option was not possible in my case but I’m really concerned about the scaring I will face from this procedure. Can a scar so large be significantly improved using any of the procedures you have mentioned?
Also while doing the hepatectomy would it make a difference in the incision itself if a plastic surgery did all the incisions and stitching versus a liver surgeon? Is that even a possibility to have a plastic surgeon do all the incisions and stitching during the surgery?
Lastly, are there any products or recommendations for care to help the healing process to aid in scarring?
Thank you so much in advance for your help!
sorry for the late reply. I assume this has all taken place by now. I would use some silicone gel on the scars for close to a year, and then consider what you want to do. Scar revision is always a possibility, but I”m more concerned with why you needed the hepatectomy in the first place.
If have a 6 year old c section scar that has a flap of skin around it it used to be smaller but since I gained weight is bigger would like to have scar revision for my flap and my scar It’s puffy and it’s extremly painful my doctor cut on the same cut twice 5 years apart I have a lot of cellulite and stretch marks in the bottom area of my stomach the top is ok can this be fixed I’m only 29 years old and I don’t want a tummy tuck
Yes, it sounds like that can be addressed surgically with a good outcome. Would love to see it though…
I got the burn scars in my face when I was 6years now I m 29 years so I need to remove i. I would like to send you the picture
okay, please send to [email protected]
Good afternoon Dr. Sterry, I have a scar in my left upper thigh and it turn purple with a big bump, is there any way for me to have this scar removed or at least for the purple bump to be even out so I can cover this scar with a tattoo. Can I send you images, so you can let me know if I am a candidate for scar revision
sure. [email protected]
I am in the process of laser tattoo removal. The removal process has not caused any scarring, but I have some raised scarring from when the tattoo was originally done. Is there anything that can be done to help those raised scars from the tattoo outline?
This question is really very specific to you. It’s probably best for you to find a board certified plastic surgeon in your area and have them examine you. Good Luck!
Hello! I’m writing because I have a 24-year-old vertical appendectomy scar that’s about 3″ long starting at the belly button. I’m mostly used to it, except it’s become increasingly indented over time and I’m concerned that it will continue to be so as I get older and put on more weight. I know it has adhesions because I later had my gallbladder removed and that surgeon said he saw adhesions. Are the appendectomy adhesions causing the indention and if so, what might you recommend? I once had a massage therapist break up very small adhesions under a knee scar and it was pretty painful so I’m hesitant to try that on my abdomen.
Thanks!
So sorry for the late reply!
First, your story is very common. Those adhesions your gallbladder surgeon was talking about are internal and are not the cause of the indentation in your scar. That said, it is a similar process. What happens is that the scar tissue can retract a little bit and create the indentation over time – especially as we age or gain weight (I have no idea what your size is). The way to fix it is to revise the scar and break up the attachments of the underside of the scar to the muscle below. Typically, I move some local subcutaneous fat (which we all have) into that area to prevent the process from happening again. Of course, the other option is to have a tummy tuck which would remove the scar completely, but that’s a whole other process.
Good Luck!
Hello. Almost 2 years ago I ended up in the hospital and needed a fasciotomy on my thigh to treat compartment syndrome. I left the hospital w/multiple scars, but one of the incisions required a skin graft to close the wound. I’m really not happy with how it looks and I am wondering if plastic surgery is an option?
Thank you!
If it’s been two years, then I imagine the swelling is much better and would bet you can remove the skin graft. That is the EXACT scenario that occurred with this patient’s arm:
https://www.drsterry.com/photo-gallery/body/scar-revision/113/36
Hi , I am 33 years old and I have a scare on my left check as result of cosmetic surgeries that was done about 10 years ago . The scar area is still not completely removed and i have also done 3 micro needling and 1 laser resurfacing session but i believe it did not help improve my scar. I would really appreciate if you could have a look at the scar as well .
send some well lit photos to [email protected]
We will reply.
Hello Dr.Sterry,
I live in NY, I am 26, and I’m scheduled to get a right hepatectomy using the Makuuchi in the next few weeks. I was told laparoscopic option was not possible in my case but I’m really concerned about the scaring I will face from this procedure. Can a scar so large be significantly improved using any of the procedures you have mentioned?
Also while doing the hepatectomy would it make a difference in the incision itself if a plastic surgery did all the incisions and stitching versus a liver surgeon? Is that even a possibility to have a plastic surgeon do all the incisions and stitching during the surgery?
Lastly, are there any products or recommendations for care to help the healing process to aid in scarring?
Thank you so much in advance for your help!
Oh my! I’m sorry, but I just saw this message from last May. I hope you recovered well from that surgery. If there is a scar that is bothersome, please give my office a call. I’d be happy to help out.
Hi I had a tummy tuck that left me with a small t scar that was raised. After injecting the raised scar I’m left with a weird indentation that looks worse when I’m sitting. It’s above the pubic area. Is this fixable? I’m worried it will look more atrophied as time goes on or if I gain weight. Would a fat transfer work in this situation?
Thanks.
I hate that “T” shaped scar thing and I have NEVER done a tummy tuck that way. I see no reason for it. Yes, a fat injection might help with the indentation – and maybe even the quality of the skin.
Good Luck!
Hi, I am fifteen years old I have had a bad burn of my left leg from hot coffee, it almost covers the front part of my thigh and little behind it too. I was wondering if you do that kinda work? I have gone to dermatologists and they all say that the scar is too large for it to be removed and that it was always stay in the same condition. It really brings my confidence and self-esteem down which I’m sure you understand. Please let me know if you can help.
Hi Ashley,
In a case like this, I would need to see the area and extent of the burn scar. Can you send a photo to “[email protected]”?